TMJ pain, jaw clenching and teeth grinding
When your jaw is working too hard, you feel it everywhere.
For some patients, it starts as jaw tension. For others, it is temple headaches, worn teeth, broken sleep, clicking, clenching, or that heavy ache around the face and ears that never quite settles. Temporomandibular disorder, often shortened to TMD, affects the jaw joint, the chewing muscles, or both. Common symptoms include pain around the jaw, ear and temple, headaches around the temples, clicking or grinding noises, difficulty opening fully, and jaw locking. Stress and clenching can make symptoms worse.
At Longwood House, we start by working out what kind of TMJ problem you actually have. That matters, because not every sore jaw needs the same treatment, and not every headache is coming from the jaw.
What is TMJ, and why does it hurt?

The temporomandibular joints are the two joints that connect your lower jaw to your skull. They do a huge amount of work every day, talking, chewing, yawning, swallowing, even holding tension when you are stressed.
TMD can be mainly muscle-based, mainly joint-based, or a mixture of both. Muscle-based problems are often linked with clenching and grinding, especially at night. Joint-based problems may come with
Signs your jaw may be involved

You may notice:
- neck and shoulder tension linked with jaw-muscle overactivity
- jaw pain, facial pain, or tenderness in front of the ear
- headaches around the temples
- clenching or grinding, especially at night
- clicking, popping, or grating from the jaw
- stiffness, limited opening, or locking
- tooth wear, tooth sensitivity, or fractured teeth from heavy pressure
Our approach at Longwood House
We do not jump straight to treatment.
We begin by listening carefully, examining the jaw, the muscles, the bite, the teeth, and the pattern of pain. Then we explain what looks muscular, what looks joint-related, and what we think is worth doing first.
For some patients, the right answer is a splint and self-management.
For some, it is restorative work to protect worn or broken teeth.
For some, where muscle overactivity is a major driver and conservative options have not been enough, prescription-only jaw-muscle relaxation treatment may be discussed as part of the plan.
Book a TMJ consultation
If your jaw feels tight, tired, painful, or “always on”, or if you keep waking with headaches, clenching, or sore chewing muscles, book a consultation. We will talk through what is happening, what type of TMJ problem it looks like, and what your options are, clearly and without rush.

How prescription-only muscle-relaxing treatment can help
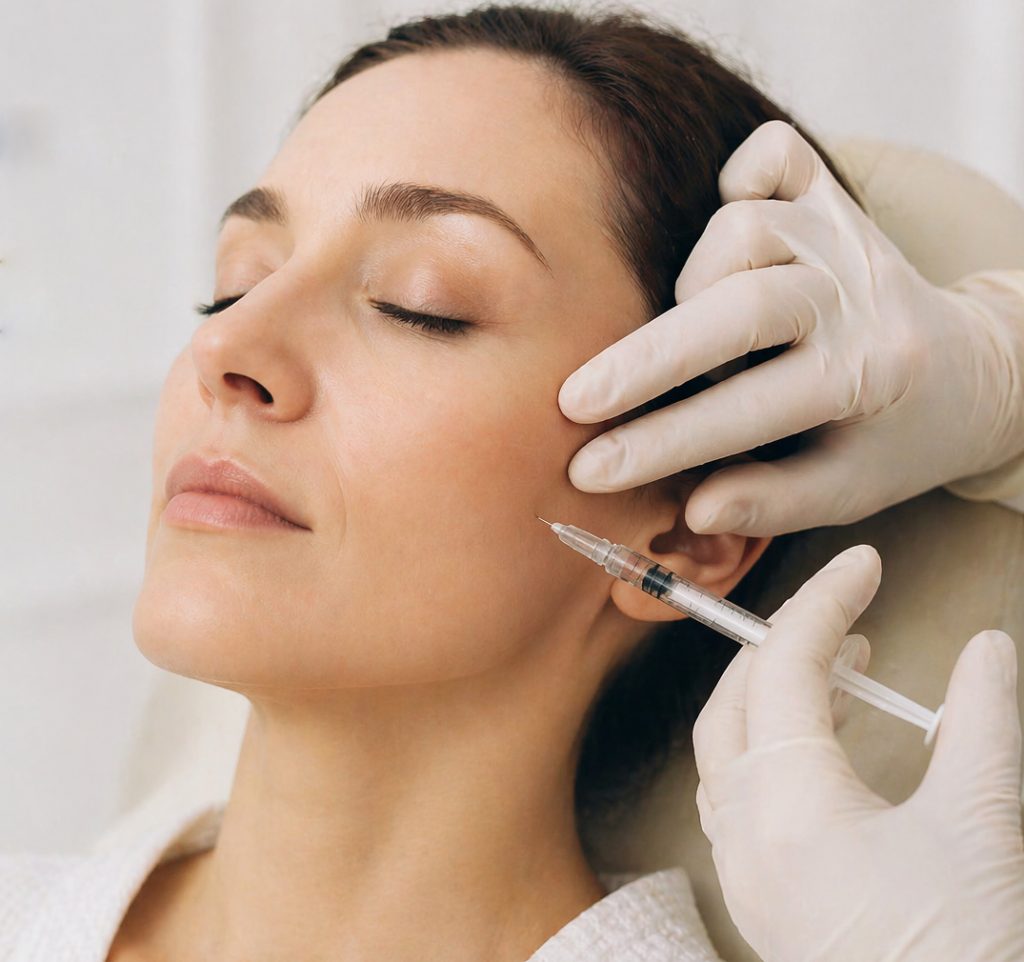
For some patients, the main problem is overactive jaw muscles. In those cases, prescription-only neurotoxin treatment can be used to temporarily relax the muscles that are overworking. Hospital guidance describes this as a way to reduce jaw pain, clenching, and muscle overactivity in selected TMJ cases.
This treatment is not a cure for every TMJ problem, and it is not first-line treatment. Current Royal College guidance says botulinum toxin A should not be first line, because the evidence is still developing, and decisions should be made carefully with informed consent and shared decision-making.
That is why we assess first. If your symptoms are mainly muscular, and if more conservative care has not helped enough, this may be one of the options we discuss. Royal Free guidance notes it may be suitable for people with jaw pain, clenching or teeth grinding that has not improved with other treatments such as physiotherapy or a mouthguard.
What treatment usually involves
The appointment itself is quick. Small amounts are placed into the muscles that need treatment, using a fine needle. Most patients describe it as tolerable, more of a brief sting than anything else. It is generally done as an outpatient treatment, so you go home the same day.
You do not usually see the full effect immediately. Early effects can start within 48 to 72 hours, with the full effect taking up to 14 days. The effect is temporary, and movement usually starts to return from around 8 to 12 weeks, although this varies from person to person.
What improvement can feel like
In the right case, patients often describe a jaw that feels less “switched on”. Less gripping. Less morning tension. Less pressure through the temples. Less soreness when chewing. Sometimes the biggest relief is not dramatic, it is simply realising the jaw is no longer dominating the day.
That said, good TMJ care is rarely about one thing alone. NHS and Royal College guidance both emphasise the importance of self-management, including softer food during flare-ups, heat or ice, massage, jaw exercises, stress reduction, and avoiding habits like gum chewing, nail biting, pen chewing, and daytime clenching. Full-coverage stabilisation splints are also commonly used in appropriate cases.
Is it safe?
These injections should only be provided after proper assessment by a trained clinician. Royal Free guidance says side effects are usually uncommon and temporary. These can include bruising, swelling or tenderness at the injection site, mild headaches, and, more rarely, temporary facial weakness or asymmetry. The same guidance says this treatment is not recommended in pregnancy, during breastfeeding, or in people with myasthenia gravis.
There is also still some uncertainty in the evidence base, including questions around who benefits most and concerns about possible bony changes with repeated treatment, which is one reason the Royal College says it should not be first line..

